Lack of Access = Lack of Power to Decide
More than 19 million women of reproductive age living in the US are in need of publicly funded contraception and live in contraceptive deserts. Living in a contraceptive desert means that they lack reasonable access in their county to a health center that offers the full range of contraceptive methods. Around 1.2 million of these women live in a county without a single health center offering the full range of methods. For all of these women getting contraception means having to do more than showing up to an appointment. They must find a babysitter, take time off work, or travel long distances to access their preferred birth control method. And they're not alone.
We know that there are women across the US who aren't eligible for publicly funded contraception but still rely on the same health centers. Whether for convenience, privacy reasons, or instances of reproductive coercion, women who have insurance may still seek contraception at health centers that primarily serve low income women. It only tells part of the story to say that 19 million women live in contraceptive deserts.
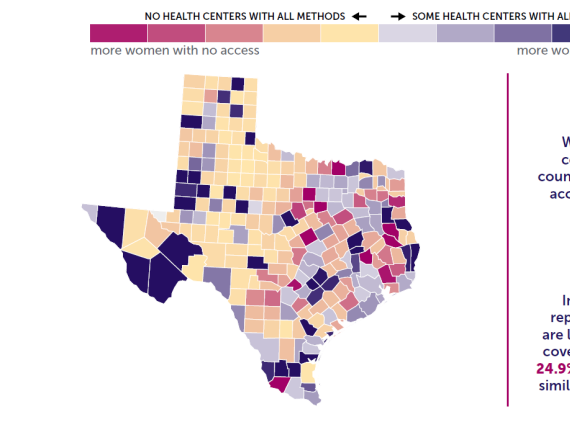
The map below provides a visual description of where women in need can access birth control—and where they can’t—across the country. As the map moves from dark purple to yellow to dark pink, access declines.
Support our work and turn this whole map purple, the colors of access and power to decide.
Why It Matters Right Now
Right now more than 19 million women in need live in contraceptive deserts. They lack reasonable access to a health center offering the full range of methods. Deep in the heart of those deserts, 1.2 million women in need live in counties without a single health center that offers the full range of contraceptive methods.
For these women seeing a provider, accessing trusted information, and finding the right birth control becomes nearly impossible.
Delilah lives in Northern Texas, a contraceptive desert. In her county and the dozen counties around her there are no health centers. To consult with her doctor about changing pill brands she must travel for nearly seven hours and go more than 400 miles to a county with two health centers.
Maya lives in a county in Arizona with eight health centers. But the wait time at each means that she needs to request an appointment three weeks in advance for a consultation. Because her preferred birth control method is an IUD, she also needed to wait a week before returning to have the IUD inserted.
Leah lives in Ohio and though she has access to a clinic, she has to take time off work to go to her appointment. With a smaller paycheck this month she has to wait to replace her car's battery so she can afford to pay her babysitter while she's at the doctor.
Beyond Definitions
It's important to understand the problem, but defining and tracking the US's contraceptive deserts is not enough. We are fighting for access on multiple levels. We won’t stop until every young person has access to accurate, quality sexual health information and the full range of contraceptive methods—without barriers or judgment. To reach that goal we're looking to answer questions such as:
- How can we encourage providers to offer the full range of contraceptive services?
- How do we fill the gaps in service in the meantime?
- How do we protect coverage as it exists right now?
- How do we ensure that everyone has access to the full range of contraceptive methods within 60 minutes of where they live?
Support our work and help women across the country receive the access they deserve.
About the Birth Control Access Map
The Birth Control Access Map depicts the availability of health centers in each county across the U.S. that provide any form of birth control, as well as the full range of methods (i.e., health centers that offer IUDs, implants, and most other FDA-approved methods such as birth control pills, the shot, the ring, the patch, cervical caps, diaphragms and emergency contraception on site).
When there are zero health centers in a county, the colors reflect the number of women in need of publicly funded contraception who live in those counties ranging from yellow (fewer women with no access) to dark pink (more women with no access). When health centers are present in a county, they are represented in shades of purple, with the darkest shade representing “reasonable access,” which is defined as at least one health center or provider that provides the full range of contraceptive methods for every 1,000 women in need of publicly funded contraception.
Download our handout on the birth control access map.
Contraceptive Deserts
Contraceptive deserts are defined as counties where the number of health centers offering the full range of methods is not enough to meet the needs of the county’s number of women eligible for publicly funded contraception, defined as at least one health center for every 1,000 women in need of publicly funded contraception. We consulted the ratios developed by Richard Cooper, MD, of the University of Pennsylvania Wharton School, one of the leading physician utilization and supply experts in the United States, in his Hospital-Specific Physician Requirements Model. Dr. Cooper’s model, developed in 2012, indicates the number of physicians in various specialties that a community can support and is “demand based.” The numbers are based on national figures and are not necessarily universally applicable, but they are among the most accurate we have to study supply and demand. Those counties with one health center per 1,000 women are shown by the darkest purple, counties with one health center per 2,000 women are shown by the middle purple shade, and those with one health center per 5,000 are shown by the lightest purple.
Data Sources
The maps include more than 16,000 health centers and providers. The data come from multiple verified sources, including Title X clinics, Planned Parenthood, and Health Resources and Services Administration, Federally Qualified Health Centers, and county and state government programs, as well as from providers who identify themselves as places for women in need to access services. Power to Decide manages this nationwide compilation of data, which also includes Puerto Rico. The vast majority of publicly funded clinic locations are included on these maps, as well as private providers and other health care sites that have made themselves known to us. Any site or provider can register its location and services. The data on the number of women in need of publicly funded contraception come from the Guttmacher Institute.
Data Limitations
We continually update our information, but the landscape of contraceptive access is constantly changing. The database has limited listings of private providers even though some private providers do accept Medicaid and could, in theory, offer the full range of methods to women in need. Further, as pharmacies become sources of direct access (without a prescription) to a wider range of contraception in the United States in places like California, Oregon, and Tennessee—and online—we will begin to build a database of those locations. However, no pharmacy or online source offers direct access to the full range, and most effective forms, of contraception—the focus of our heat maps.
Access View Limitations
The current view is only one way of looking at access: by the proximity of health centers and the availability of the full range of contraceptive methods for women in need of publicly funded contraception. The color chart doesn’t depict the population of women who are not in financial need of or eligible for publicly funded contraceptive services and supplies, yet may still need to rely on such health centers. Included in this group are women who may not want to use their insurance for privacy reasons or who travel to a location out of their area to hide their contraceptive from their partner—an all-too-common story—so as to avoid birth control sabotage or coercion.
Many other barriers can stand in the way of a person’s access, and we would like to represent those in the future, including lack of same-day service, cost, unavailability of a same-gender provider, lack of a pleasant environment, or a poor customer service rating. In addition, our current view of proximity is limited in that it does not represent one’s ability to access transportation to get to a health center or pharmacy. In many areas of the country, a high percentage of people lack access to a vehicle or other form of transportation, thus making more important the availability of close-by health centers and pharmacies. In addition, people who cannot afford health care and who often are missing from the system face knowledge gaps, which represents another kind of access barrier. Often people in this cohort go to a local pharmacist to ask questions about a wide range of health issues, but in many areas of the country getting to a pharmacy, or any provider, to ask a question is difficult. We seek to represent this lack of access on a map in the future.